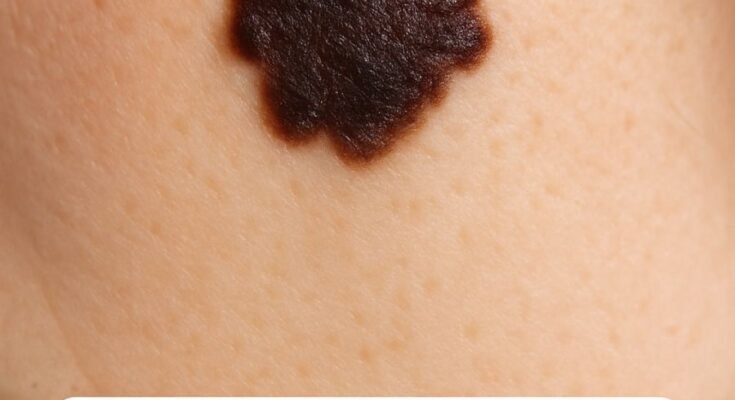
Moles are common skin growths that most people have on their bodies. Typically benign, they can vary in color, shape, and size. However, it’s not uncommon for people to become concerned when they notice changes in their moles, especially when those changes happen suddenly. One such change that often raises alarm is when the edges of a mole become jagged or irregular.
While the appearance of jagged edges in a mole can be unsettling, it’s important to approach the situation with calm and informed action. In this article, we delve into the potential implications of such changes and provide guidance on how to proceed when your dermatologist is not immediately available.
1. Why Sudden Jagged Edges on a Mole Deserve Your Attention
Moles can change for a variety of reasons, and not all changes are cause for alarm. However, sudden changes in the appearance of a mole, particularly its edges, should be monitored closely. This is because one of the warning signs of melanoma, a type of skin cancer, is an irregular or notched border. While not every change indicates cancer, it’s important to err on the side of caution.
If the jagged edges are accompanied by other changes such as color variation, an increase in size (greater than 6 millimeters), or the mole becoming elevated, it’s crucial to document these changes and seek medical advice promptly, as these can be indicative of atypical cells.
2. The ABCDE Rule: A Quick At-Home Check for Dangerous Moles
The ABCDE rule is a helpful guide for identifying potentially dangerous moles. ‘A’ stands for Asymmetry, where one half of the mole doesn’t match the other. ‘B’ refers to Border irregularity, such as jagged or blurred edges. ‘C’ represents Color variation, with multiple colors or shades within a single mole. ‘D’ stands for Diameter, where moles larger than 6mm should be watched closely. ‘E’ signifies Evolving, any change in size, shape, color, or symptoms such as itching or bleeding.
By using the ABCDE rule, individuals can perform a preliminary check at home to assess the potential risk of a mole. This method can provide peace of mind or indicate the need for prompt medical evaluation.
3. What Is a Dysplastic Nevus and How Is It Different From a Normal Mole?
A dysplastic nevus, also known as an atypical mole, is a mole that looks different from a common mole. These moles can be larger than ordinary moles, often more than 5mm across, and may have a mixture of colors and irregular borders. While having a dysplastic nevus does not mean you have cancer, it can increase your risk of developing melanoma.
In contrast, normal moles are usually uniform in color, round or oval in shape, and no larger than a pencil eraser. Recognizing the difference between typical moles and dysplastic nevi can be crucial in early detection of potential skin cancers.
4. When a Dysplastic Nevus Can Turn Into Melanoma (and When It Usually Doesn’t)
Dysplastic nevi are more likely to develop into melanoma compared to normal moles. However, the majority of these moles do not turn into cancer. The risk of melanoma increases with the number of dysplastic nevi present on the body, especially if there is a family history of melanoma.
Regular monitoring of dysplastic nevi is important. If a dysplastic nevus begins to change in appearance, it should be evaluated by a healthcare professional as soon as possible to rule out the possibility of melanoma.
5. Red-Flag Changes: Edges, Color, Size, and Other Warning Signs
Changes in a mole’s edges, such as becoming jagged or notched, can be a red flag for melanoma. Additional warning signs include color changes, particularly if the mole turns darker or has multiple colors; an increase in size, especially if it exceeds 6mm; and any new symptoms like itching, tenderness, or bleeding.
It’s important to be vigilant about these changes, as early detection of melanoma can significantly improve treatment outcomes. Document any changes and seek medical advice if you notice multiple warning signs.
6. Common Benign Reasons a Mole’s Border Might Look Weird Overnight
There are benign reasons why a mole might appear to change overnight. Trauma to the mole, such as scratching or bumping it, can cause temporary inflammation and changes in appearance. Hormonal changes or exposure to sunlight can also affect moles.
While these changes can be harmless, it’s important to monitor the mole and ensure that it returns to its usual appearance. If the changes persist or worsen, consult a healthcare professional.
7. Viral Skin-Check Hacks: What Actually Helps and What to Ignore
In the age of social media, various skin-check hacks circulate online. While some may offer practical advice, others can be misleading. It’s important to rely on proven methods, like the ABCDE rule, rather than DIY remedies or unverified hacks.
Photographic apps and online guides can be useful for tracking changes, but they should not replace professional medical advice. Always verify information with trusted medical sources and consult a healthcare provider for concerns.
8. What Never to Do: Popping, Picking, Freezing, or DIY Mole Removal
Attempting to remove or alter a mole at home can lead to infection, scarring, and potentially mask symptoms of skin cancer. Popping, picking, or freezing a mole is not advisable and can cause more harm than good.
Professional evaluation and treatment are crucial for any suspicious mole. Dermatologists have the expertise to safely assess and, if necessary, remove moles while minimizing risks and ensuring proper diagnosis.
9. Step-by-Step: How to Photograph and Track a Changing Mole at Home
Taking clear photographs of a changing mole can be a valuable tool for monitoring its progression. Use a ruler or a coin for scale and ensure the lighting is consistent in each photo. Take pictures from multiple angles and store them in a designated folder for easy comparison.
Track any additional changes such as new symptoms or alterations in color and size. This documentation can be helpful when discussing your concerns with a healthcare provider.
10. How Urgent Is This? Deciding Between ER, Urgent Care, and Waiting for Dermatology
Determining the urgency of a mole change depends on the severity and accompanying symptoms. If the mole is bleeding, rapidly changing, or has other concerning signs, visiting urgent care or the ER might be necessary.
If the changes are less severe but still concerning, scheduling an appointment with a dermatologist should be prioritized. If immediate care is unavailable, request to be placed on a cancellation list or ask for telehealth options.
11. What to Say When You Call the Doctor: Getting an Earlier Appointment
When calling your dermatologist, be clear and concise about your concerns. Mention specific changes such as jagged edges, color variations, or symptoms like itching or bleeding. Stress the urgency of the situation based on these observations.
Request to be added to a cancellation list if an earlier appointment is not available. Provide your contact information and availability for a potential last-minute opening.
12. How Dysplastic Nevi Are Diagnosed and Treated Once You’re Seen
Upon examination, a dermatologist may perform a dermatoscopic evaluation of the mole. If the mole appears suspicious, a biopsy may be conducted to determine if dysplastic cells are present.
Treatment typically involves regular monitoring and, if necessary, surgical removal of the mole. The dermatologist will advise on follow-up care and any additional steps needed based on the biopsy results.
13. Lowering Your Future Risk: Sun Protection and Regular Skin Checks
Protecting your skin from UV radiation is crucial in reducing the risk of melanoma. Use broad-spectrum sunscreen with an SPF of 30 or higher, wear protective clothing, and avoid peak sun hours when possible.
Regular self-examinations and professional skin checks are also important in early detection of any new or changing moles. Staying vigilant and proactive can significantly reduce the risk of skin cancer